Imagine standing up from your favorite chair and feeling a sudden, sharp catch in your lower back. It’s not just a twinge; it feels like something has shifted out of place. For millions of people, this isn’t a one-off incident but a chronic reality known as spondylolisthesis, a condition where one vertebra slips forward over the one below it. This slippage creates mechanical instability that can lead to persistent pain, stiffness, and even nerve damage if left unchecked. While many live with mild cases without knowing it, those with symptomatic slips face a difficult choice: manage the pain conservatively or commit to spinal fusion surgery.
The decision to undergo surgery is rarely simple. It involves weighing the risks of living with instability against the recovery demands of a major procedure. Understanding the mechanics of the slip, the severity of your symptoms, and the specific types of fusion available is crucial for making an informed choice about your spine health.
Understanding the Slip: What Is Spondylolisthesis?
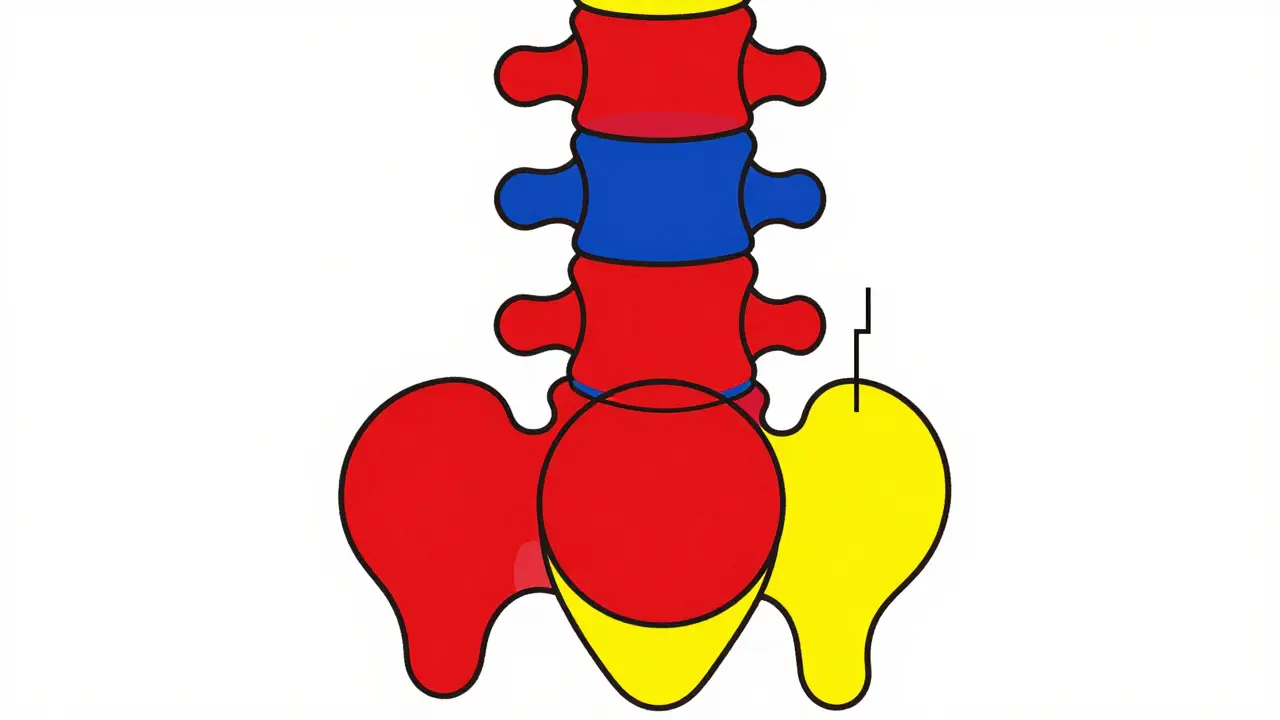
To grasp why spondylolisthesis causes such significant discomfort, you first need to visualize the spine’s structure. The spine consists of stacked bones called vertebrae. Between these bones are discs that act as shock absorbers. Normally, ligaments and joints keep each vertebra aligned perfectly over the next. In spondylolisthesis, this alignment fails. One vertebra slides forward relative to the one beneath it.
This condition most frequently occurs in the lower back, specifically between the fifth lumbar vertebra (L5) and the first sacral bone (S1). This area bears the most weight in the body, making it prone to stress. Doctors classify the severity of the slip using the Meyerding Classification system. This system grades the slip based on how far the vertebra has moved:
- Grade I: Less than 25% slippage.
- Grade II: 25% to 50% slippage.
- Grade III: 50% to 75% slippage.
- Grade IV: 75% to 100% slippage.
- Grade V: Complete dislocation (spondyloptosis), which is rare.
Not everyone with a slip experiences pain. Approximately 6% of the general population has spondylolisthesis, yet only a fraction develop symptoms. However, when symptoms do appear, they can significantly impact daily life. The pain often mimics a muscle strain but persists longer and worsens with activity, particularly standing or walking. Bending forward usually provides relief because it reduces the pressure on the slipped segment.
Why Does the Vertebra Slip? Types and Causes
Spondylolisthesis isn’t a single disease; it’s a structural result of various underlying issues. Identifying the type helps determine the best treatment path. There are five main categories:
- Degenerative: This is the most common type in adults over 50, accounting for about 65% of cases. It results from arthritis and wear-and-tear on the spinal joints and discs. As the disc height decreases, the vertebrae become less stable and can shift.
- Isthmic: Common in younger patients and athletes, this type stems from a defect or fracture in the pars interarticularis, a small bridge of bone connecting the upper and lower parts of the vertebral arch. Repetitive hyperextension, such as in gymnastics or football, can cause stress fractures here.
- Traumatic: Caused by acute injury, such as a car accident or fall, leading to fractures in the pedicle or lamina.
- Dysplastic: A congenital condition present at birth where the facet joints are malformed, allowing excessive movement.
- Pathologic: Resulting from bone weakness due to tumors, infections, or diseases like osteoporosis.
For instance, a young gymnast might develop isthmic spondylolisthesis due to repetitive backbends, while a 60-year-old teacher might develop degenerative spondylolisthesis after decades of normal aging processes wearing down their discs. The cause dictates whether the spine is inherently unstable or if the instability is progressive.
Recognizing the Symptoms: More Than Just Back Pain
If you have spondylolisthesis, your symptoms will likely evolve over time. Initially, you may notice tightness in your hamstrings, affecting about 70% of symptomatic patients. This tightness often leads to a characteristic posture change: an increased swayback (lordosis) to compensate for the forward slip. Over time, this compensation can fail, leading to a rounded back (kyphosis) in advanced cases.
Pain patterns are distinct. Unlike typical mechanical back pain that improves with rest, spondylolisthesis pain often flares up during activities that extend the spine, such as standing still or walking uphill. Sitting or bending forward typically relieves the tension. In more severe cases (Grade III-IV), the slipping vertebra can compress nearby nerves. This leads to radiculopathy, characterized by tingling, numbness, or weakness radiating down the legs. Some patients experience neurogenic claudication, a condition where leg pain and fatigue force them to stop walking after short distances.
Diagnosis requires imaging. Standing lateral X-rays are the gold standard for measuring the degree of slippage. CT scans provide detailed views of the bony anatomy, useful for identifying pars defects. MRI scans are essential for evaluating soft tissue, disc degeneration, and nerve compression. These images help surgeons decide if conservative care is sufficient or if surgical intervention is necessary.

Conservative Management: Can You Avoid Surgery?
Before considering fusion, most doctors recommend a trial of conservative management lasting 6 to 12 months. This approach aims to stabilize the spine through muscular support and reduce inflammation. Key components include:
- Physical Therapy: Core strengthening is vital. Strong abdominal and back muscles act as a natural corset, stabilizing the slipped segment. Hamstring stretching is also critical to relieve posterior chain tension.
- Activity Modification: Avoiding activities that involve heavy lifting or extreme back extension can prevent worsening the slip.
- Pain Management: Non-steroidal anti-inflammatory drugs (NSAIDs) help manage pain and swelling. In some cases, epidural steroid injections may provide temporary relief by reducing inflammation around compressed nerves.
However, conservative care has limits. If you have high-grade slippage (Grade III or higher) or progressive neurological deficits, physical therapy alone may not suffice. Studies show that patients with high-grade slips have a 68% likelihood of developing neurogenic claudication compared to only 22% in low-grade slips. In these scenarios, delaying surgery can lead to permanent nerve damage or irreversible deformity.
Spinal Fusion: The Surgical Solution
When conservative measures fail, spinal fusion becomes the primary surgical option. The goal of fusion is to eliminate motion at the painful segment by joining two or more vertebrae together into a single solid bone. This stops the slippage and prevents further nerve irritation.
There are three main approaches to spinal fusion for spondylolisthesis:
| Technique | Description | Success Rate | Best For |
|---|---|---|---|
| Posterolateral Fusion | Bone graft placed on the back of the spine along the transverse processes. | 75-85% (Grade I-II) | Mild to moderate slips with intact discs. |
| Interbody Fusion (TLIF/PLIF) | Cage filled with bone graft inserted between vertebrae to restore disc height. | 85-92% (All Grades) | Severe slips, nerve compression, loss of disc height. |
| Minimally Invasive Fusion | Smaller incisions, less muscle disruption, similar hardware. | Similar to open techniques | Patients seeking faster recovery, selected cases. |
Posterolateral fusion is the traditional method, accounting for about 55% of procedures. It involves placing bone graft material on the outer edges of the vertebrae. While effective for mild slips, it doesn’t directly address disc collapse or nerve compression as well as interbody techniques.
Interbody fusion, including Transforaminal Lumbar Interbody Fusion (TLIF) and Posterior Lumbar Interbody Fusion (PLIF), is increasingly preferred for spondylolisthesis. By inserting a cage between the vertebrae, surgeons restore disc height, open up the neural foramen (where nerves exit), and improve stability. This technique boasts higher success rates, especially for Grade III-IV slips, because it directly corrects the alignment and decompresses the nerves.
Recent advancements include the use of bone morphogenetic protein (BMP) and stem cell therapies to enhance bone growth. A 2023 multicenter trial showed BMP-2 increased fusion rates to 94% in high-risk patients compared to 81% with traditional autograft. Additionally, minimally invasive techniques allow for smaller incisions, reduced blood loss, and shorter hospital stays, though long-term outcomes remain comparable to open surgeries.
Risks, Recovery, and Long-Term Outlook
Spinal fusion is major surgery, and it comes with risks. The most significant concern is pseudoarthrosis, or non-union, where the bones fail to fuse properly. Smokers face a 3.2 times higher risk of pseudoarthrosis, making smoking cessation before surgery critical. Obesity (BMI >30) also increases complication risks by 47%. Other potential complications include infection, nerve injury, and blood clots.
Recovery is a marathon, not a sprint. Post-surgery, you’ll likely spend 6-8 weeks with restricted activity, avoiding bending, lifting, or twisting. Physical therapy resumes after this initial healing phase, continuing for 3-6 months. Full recovery, where you return to all normal activities, can take 12-18 months. Patient satisfaction rates hover around 78-85% at two-year follow-ups, indicating that most people find significant relief from pain and improved function.
However, fusion isn’t without long-term trade-offs. By immobilizing one segment, adjacent levels of the spine bear more stress. This can lead to adjacent segment disease, where the discs above or below the fusion degenerate prematurely. About 18-22% of patients develop this within five years, potentially requiring revision surgery. Revision rates for Grade III-IV slips are approximately 12-15%, highlighting the importance of careful patient selection and realistic expectations.
Making the Right Choice for Your Spine
Deciding on fusion surgery requires a balanced view of your current quality of life versus the recovery journey ahead. If you have mild symptoms and a low-grade slip, conservative care is usually the best first step. But if you’re experiencing progressive nerve damage, severe pain that limits daily activities, or high-grade instability, surgery may offer the best chance for long-term relief.
Consult with a spine specialist who can evaluate your specific anatomy, symptom profile, and lifestyle goals. Ask questions about the surgeon’s experience with interbody fusion, their success rates, and what post-operative rehabilitation looks like. Remember, the goal isn’t just to fix the slip-it’s to restore your ability to live comfortably and actively.
Is spondylolisthesis curable without surgery?
The structural slip itself cannot be reversed without surgery. However, many people manage symptoms effectively with physical therapy, core strengthening, and lifestyle modifications. Conservative care is successful for a majority of patients with low-grade slips (Grade I-II) who do not have neurological deficits.
How long does recovery from spinal fusion take?
Initial recovery involves 6-8 weeks of restricted activity. Physical therapy continues for 3-6 months. Full recovery, including returning to strenuous activities, typically takes 12-18 months. Individual timelines vary based on age, overall health, and adherence to post-op instructions.
What are the signs that I need surgery for spondylolisthesis?
Key indicators include persistent pain despite 6-12 months of conservative treatment, progressive neurological symptoms (numbness, weakness, loss of bowel/bladder control), high-grade slippage (Grade III-IV), or inability to perform daily activities due to pain or instability.
Can smoking affect my spinal fusion success?
Yes, significantly. Smokers have a 3.2 times higher risk of pseudoarthrosis (non-union), where the bones fail to fuse. Surgeons strongly recommend quitting smoking at least 4-6 weeks before surgery to optimize blood flow and bone healing.
What is adjacent segment disease?
Adjacent segment disease occurs when the spinal segments above or below a fused area degenerate faster than usual due to increased stress. It affects 18-22% of patients within 5 years post-fusion and may require additional surgery if it causes significant pain or instability.